What is hypoxia and what effects can a newborn have? Symptoms and treatment
The value of oxygen for the human body is great. Without it, existence itself will become impossible. We need oxygen and babies who are still developing in the womb. If for some reason the baby receives less oxygen than it needs, if the state of oxygen starvation develops during childbirth, then this can have quite serious long-term consequences for the health of the baby. In this material, we will talk about what constitutes hypoxia in newborns, how dangerous it is and what should be the treatment for infants.
Special features
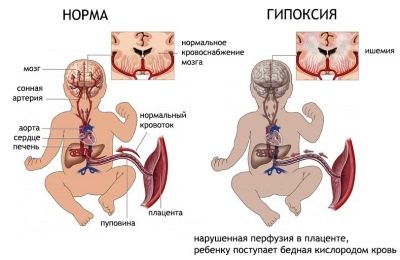
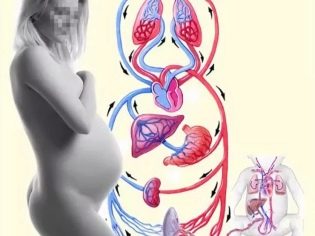
Hypoxia in medicine is called the state of oxygen deficiency. Fasting because of it can various organs and tissues of the body of the child. The brain and nervous system are most susceptible to oxygen starvation. During pregnancy, the baby receives oxygen from the mother's blood through uteroplacental blood flow. During this period, chronic hypoxia can develop if the crumb systematically loses the necessary substance.
If the pregnancy was completely normal, then no one can guarantee that hypoxia will not occur during childbirth. But then it will be called acute hypoxia.
What happens to a baby if he lacks O2? During the period of prenatal development, the baby can withstand this unfavorable factor for quite a long time - it calms down, "saves" oxygen, its movements become slower and rare. The adrenal cortex stimulates the more active work of the tiny heart. But the fetal compensatory abilities of the fetus are not infinite. If the state of hypoxia is long and severe, the baby may die.
The consequences of intrauterine hypoxia, which is most often referred to when the appropriate medical verdict is given to a newborn, can be very diverse. If during pregnancy the baby chronically lacked oxygen, it is usually born with insufficient weight, has low Apgar scores and a lot of problems with the development of the nervous system. The consequences of acute hypoxia that occurred during childbirth can be even more devastating for the baby.
In addition, in medicine there are several types of hypoxia, which mainly describe its mechanism. So, there are such subspecies as:
- respiratory - oxygen deficiency in the newborn is associated with bronchospasm or pulmonary edema;
- circulating - lack of oxygen organs and tissues of the crumbs are experiencing due to violations in the work of the heart and blood vessels;
- hemic - deficiency based on severe anemia;
- fabric - oxygen deficiency, based on the violation of the process of absorption of matter by the tissues of organs;
- combined - the lack connected with simultaneous coincidence of several factors, including pre-natal or generic.
The reasons
No baby is immune from hypoxia. It is enough to familiarize yourself with the common causes of this condition to understand that oxygen deficiency can occur at any stage of pregnancy or childbirth, as well as in the early neonatal period.
So, in the period of carrying a baby, a pregnant woman can hear from an obstetrician-gynecologist, who is observing her, that he suspects signs of hypoxia in a child. This is especially likely under the following circumstances:
- the presence of diabetes in women;
- infectious diseases that a woman had had during the first trimester;
- multiple pregnancy;
- long-standing threat of miscarriage;
- placental abruption;
- prolonged pregnancy (childbirth after 42 weeks);
- insufficient levels of hemoglobin in the blood of the future mother;
- pathology of the placenta, umbilical cord, impaired blood flow between the mother and baby;
- smoking, drinking alcohol;
- rhesus conflict
During childbirth, a state of acute hypoxia can develop, in which the baby will experience a serious shock. Such deficiency may result from:
- rapid, rapid delivery;
- a long anhydrous period with premature discharge of amniotic fluid;
- asphyxia umbilical loops during entanglement, pinching the umbilical cord loop with impaired blood flow;
- childbirth on the background of polyhydramnios or low water;
- natural childbirth in multiple pregnancies;
- too early placental abruption (before the birth of the baby);
- weakness of generic forces.
Early neonatal hypoxia most often develops in premature babies with low body weight, immature lung tissue, and metabolic disturbances.
Signs of
Hypoxia in the fetus during pregnancy is diagnosed with great difficulty, because The only way to detect anxious symptoms is to count fetal movements. If the crumb suddenly activated, his tremors became very frequent, sometimes painful for the woman, with a high degree of probability he is experiencing a state of oxygen starvation. With his movements, he tries to pull at the placenta in order to extract a little more than the substance it needs. In the state of prolonged hypoxia, fetal movement, on the contrary, slows down, becomes rare and sluggish.
Such complaints to a pregnant woman are the basis for an unscheduled ultrasound, with a doppler, in order to assess the speed and volume of blood flow in the mother-placenta-fetus system. At a gestational age of 29 weeks gestation, CTG - cardiotogram can be performed. But all these methods can only indicate a certain unfavorable condition of the fetus in the womb, but to answer the question whether there is hypoxia exactly, they, alas, cannot.
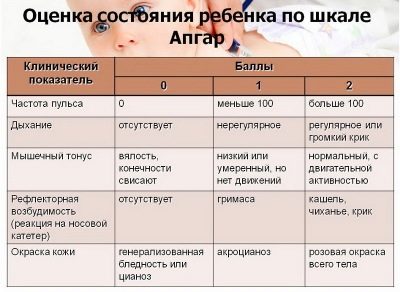
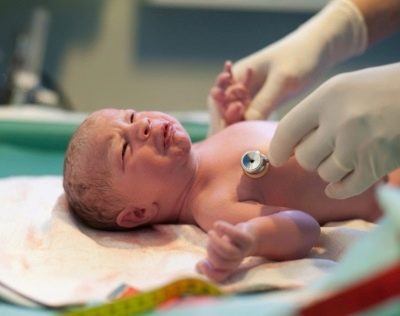
The state of acute hypoxia is determined during childbirth, if the birth process occurs under the control of CTG. Doctors neonatology, examining the baby, note the effect of hypoxia on his condition, and this is reflected in the Apgar score. A baby who has experienced prolonged hypoxia in the womb or who has experienced it during the period of birth usually does not immediately cry, his skin is bluish. Often the child requires the help of resuscitators.
In the early neonatal age, signs of hypoxia are manifested in the restless behavior of the baby and the numerous neurological symptoms that are visible not only to the neurologist, but also to the mother, who is completely far from medicine. Such children often and for no apparent reason cry and scream, arch the back of the arch and at the same time throw back the head, they have abundant and frequent regurgitation, disturbed sleep and appetite, can be pronounced tremor of the limbs and chin, nystagmus pupils of the eyes.
The exact list of disorders depends on which part of the brain suffered most from oxygen starvation. A mild form of hypoxia can not cause external symptoms, only an experienced doctor can see small "problems" and "inconsistencies" in development. Hypoxia 2 degrees most often becomes the cause of coronary disease, but this is not always a danger in the future.
Hypoxia of moderate severity and severe form are dangerous. Violations can be noticeable almost immediately. These are various forms of paralysis and paresis, cerebral palsy, encephalopathy, severe damage to the organs of sight, hearing, speech centers and the musculoskeletal system.
Very often, an increased muscle tone in a newborn is “recorded” in the symptoms of hypoxia.It is easier for the doctor to explain to the mother that the tone is a consequence of a lack of oxygen, to appoint a massage, than to tell that tone is a normal phenomenon for all newborns without exception. However, a generalized hypertonus that covers all muscle groups of a baby cannot be considered physiological at all. It may be a consequence of postponed hypoxia.
On the question of whether hypoxia affects the development of the baby, the answer is always affirmative. The only question is how big are the post-hypoxic changes in brain structures. A slight hypoxia, subject to the recommendations of the doctor may not have a significant effect on the crumbs. It is difficult to speak about severe hypoxia, which was complicated by oxygen starvation and the subsequent death of brain cells. The consequences will be how much cell loss is.
Therapy
If the state of oxygen starvation of the fetus is detected before birth, the treatment is carried out by an obstetrician-gynecologist. It includes hospitalization in the hospital, the introduction of drugs that improve blood circulation in the "mother-placenta-fetus" system, iron preparations are shown to increase hemoglobin level, vitamins, magnesia for removal of uterine tone.
If the therapy is unsuccessful, the decision is made on early delivery, since further gestation and prolongation of pregnancy are regarded as a dangerous condition for the life of the child.
In acute hypoxia, which developed during childbirth, help is provided to the baby in an emergency mode. In the birth room invite resuscitator. The baby is placed in a special resuscitation box, provide a constant access of oxygen through the imposition of an oxygen mask.
Additionally introduced drugs that improve blood circulation, sedatives. An examination of the state of the brain is carried out on the first day after birth. Further treatment while in the hospital depends on the extent of the damage. After hypoxia, the mother and child will not be discharged home, they will be sent to treat the effects of oxygen starvation in the children's hospital.
The recovery from the experienced hypoxia is rather long. To this parents need to prepare. After inpatient treatment will continue at home. The child will be put on a dispensary account to a neurologist. To visit this doctor will need to be no less than the district pediatrician.
Monthly child must be examined for ultrasound, conduct neurosonography, then ultrasound of the brain (through the fontanelles on the head) do as needed at the age of one year. After that, EEG, Echo EG, MRI or CT can be prescribed for suspected cysts, tumors, extensive damage to the central nervous system.
The standard course of treatment includes massage, daily gymnastics, swimming, compulsory walks in the fresh air, and physiotherapy. If medicines are prescribed, the mother’s task is to ensure that the child receives the medicines regularly and in the recommended dosage. Children with posthypoxic changes are recommended long-term breastfeeding (at least up to a year), hardening and cool bathrooms, compulsory vaccination against common dangerous ailments according to the National Immunization Schedule.
In a family where a baby is born, who was born with signs of hypoxia, there must be a normal psychological climate, this is very important in view of the increased nervous susceptibility of the baby. It is necessary to limit visits to guests, relatives, and noisy companies, the child necessarily needs a sparing day regimen and the absence of stressful situations.
Opinion of Dr. Komarovsky
A well-known pediatrician and TV presenter, author of books on children's health, Yevgeny Komarovsky, is often forced to answer parents' questions about the possible consequences of hypoxia suffered by an infant. He believes that the most important role in the treatment of the child is performed by non-neurologists and pediatricians, not expensive medicines, regular massage and visits to doctors.
Neurologists often make mistakes, diagnostics is not 100% accurate, and medications standardized for children after hypoxia, in general, according to Komarovsky, raise serious doubts, because the benefits of vitamins and vascular drugs in the process of restoring brain cells are minimal.
He treats a child for the love and care of parents, developmental activities with the participation of a qualified child psychologist, participation in the life of the baby. Without this, forecasts for the future, says Komarovsky, are very, very unfavorable.
In most cases, with mild and moderate hypoxia, everything goes without serious consequences. The main thing is not to panic and do not rush to extremes. It is the extremes of Komarovsky that are considered the most dangerous consequence of oxygen starvation. Neurologists exaggerate the consequences, and sometimes even do overdiagnosis - a tremor in the chin while sucking the pacifier or an increased tone of hypoxia, according to Komarovsky, do not speak. However, parents are persistently prescribed examinations and expensive massage courses, without which the baby can do in 95% of cases, limiting himself to mother's home massage without significant financial costs.
Parents, according to Komarovsky, are too trusting and prone to alarmism, and therefore they agree on everything - popular methods, osteopaths, manual therapists, Voodoo and the ritual of removing damage, just to save the kid from such dangerous and prescribed effects of oxygen starvation by the doctor. This approach sometimes harms the child more than the hypoxia itself.
Parent reviews
In the opinion of many mothers, doctors really do not stint on making such a diagnosis, as a result, almost every second newborn gets a referral to a neurologist and a massage. But now, mothers more often refuse and choose the approach that Komarovsky adheres to - which are recommended to be taken to restore the brain - they are treated with love, care and adequate care.
The most difficult thing, according to moms, is to survive a period of complete uncertainty, when no doctor can give any predictions as to whether any effects of oxygen starvation will manifest. Moms have to be more attentive, observant and develop analytical skills in order to notice deviations and anomalies in the baby’s behavior in time.
Many mothers note that swimming has a positive effect on the child’s condition from a very young age. Symptoms of neurological disorders quickly passed and by the year the neurologist who had observed the child admitted that the situation had changed for the better.
Most parents note that up to 3 years in children who have suffered hypoxia, speech develops more slowly, but by 5-6 years all defects can be corrected. Complaints that a teenager speaks poorly or understands little after hypoxia experienced in childhood does not occur on the forums.
For the prevention of fetal hypoxia in a pregnant woman, see the following video.