Respiratory rate in children: the norm by age
Not only pulse, temperature and arterial pressure can tell a lot about a child’s condition. A very informative indicator is considered and the frequency of respiratory movements. How to learn to measure it, and what frequency is considered the norm, we will tell in this article.
What it is?
Such a biomarker, as the frequency of respiratory movements, has been known since ancient times. The healers of the ancient world noticed that this indicator changes in a sick person. Today, the NPV (respiratory rate) does not lose its relevance in the diagnosis of a wide variety of childhood and adult diseases. One movement is considered to be one series of "inhale-exhale". Estimated number of such movements for a specific period of time - usually 1 minute.
It should be noted that The NPV in children is not at all similar to that in adults. Children, because of their anatomical features, breathe a little differently - their breathing is shallow, shallow, the frequency of inhalation and exhalation is much higher. The need for oxygen in a growing child's body is extremely high, and the volume of the lungs and the size of the chest is small. That is why the baby needs intensive breathing.
However, there are certain standards for different ages. And the excess breathing rate in excess of these norms may indicate that the child has oxygen starvation (hypoxia). Rapid breathing accompanies a wide variety of pathologies in children.
Why measure?
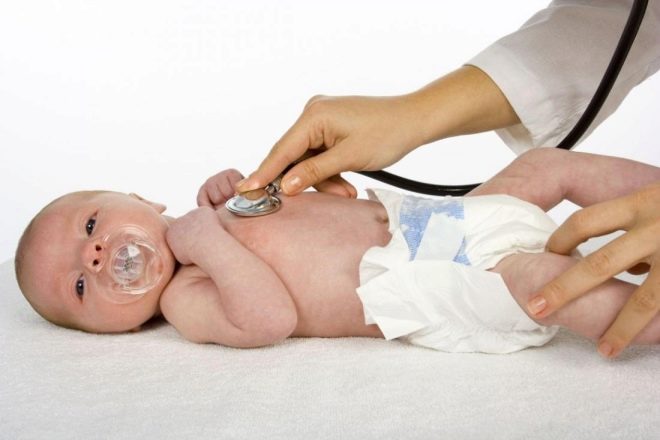
The frequency of respiratory movements, coupled with the determination of heart rate and type of breathing, is of paramount diagnostic importance when examining a newborn and an infant. Such children cannot tell their parents what exactly worries them, and only from the NPV indicators one can understand that something is wrong with the crumb. Most of the diseases that are accompanied by rapid breathing in children are successfully treated. with timely treatment and the provision of proper medical care. The pediatrician, of course, will pay attention to the child's NPV at each scheduled visit to the clinic.
The rest of the time, parents are on guard of children's health; they must be able to distinguish between normal and abnormal breathing.
It is not difficult to do this, the frequency of respiratory movements is a parameter that any mother, any father and grandmother of the baby can independently determine. The main thing is to do everything correctly and correctly evaluate the results.
How to measure?
If it seems to parents that the child breathes too often, the frequency of breathing should be measured. It is best to do this when the child is calm, for example, in a dream. When a pussy stays awake, plays, experiences something, experiences emotions, breathing becomes more frequent, and it is quite natural.
Mom should put her hand on the chest or belly of the child. The choice of location of the measurement is very important, because it determines the type of breathing of the baby. In infants and children up to 4-5 years, diaphragmatic breathing prevails (the child breathes with the abdomen, the peritoneum on the inhale methodically rises, and at the exit it lowers).
At the age of 4, the development of a new way for the baby to breathe begins - chest breathing (when the chest cell rises and falls when making inhalation and exhalation). By the age of 10, the child forms the type that is more peculiar to him by gender. In boys, abdominal breathing is usually observed, and in girls - diaphragmatic. Thus, it is very easy to determine where to put your hand. need to build on the age of the child.
The counting algorithm is pretty simple. Within 1 minute, consider the breath in and out episodes. One series of such movements is considered for one respiratory movement. Big mistake to measure the breath for 30 seconds, then multiply the resulting number by two. Breathing is not as rhythmically as, for example, pulse, and therefore such a simplified method for measuring NPV is not suitable. One more minute the parents will spend on measuring the heart rate (pulse) and it will be possible to assess the condition of the child, starting from the age norms.
An electronic watch, stopwatch, or a watch with an arrow will be useful for measuring.
Norms
There are a lot of tables on the Internet, according to which it is proposed to compare the data obtained as a result of measuring the child’s respiratory rate with the norms. It is difficult to assess the veracity of each. Pediatricians try to adhere to data that is published in Berkowitz s Pediatrics: A Primary Care Approach. They are officially recognized:
- Newborns. Respiratory rate - 30-60 times per minute. Pulse - from 100 to 160.
- Children 6 months. Respiratory rate - 25-40 times per minute. Pulse - from 90 to 120.
- Children in 1 year. Respiratory rate 20-40 times per minute. Pulse - from 90 to 120.
- Children in 3 years. Respiratory rate 20-30 times per minute. Pulse - from 80 to 120.
- Children in 6 years. Respiratory rate 12-25 times per minute. Pulse - from 70 to 110.
- Children in 10 years. Respiratory rate - 12-20 times per minute. Pulse - from 60 to 90.
Attentive parents will be able to notice any deviation from the individual children's norm. We are talking about the frequency at which the child usually breathes, because one baby has 40 breaths in 60 seconds, and another baby at the same age has only 25. It is clear that in the second case the frequency will increase to 40-45 considered to be a violation, and in the first, the crumbs with frequent breathing from birth, the same indicators will be the norm. Parents should not ignore their own observations. After all, moms and dads know better the individual characteristics of their baby than anyone, even a very good doctor, who sees a child for the first time.
Reasons for rejection
The excess frequency of respiratory movements in medicine is called Tachypnea. This is not a disease, but only a symptom that can speak about the development of a specific pathology. You can talk about tachypnea in the event that if the NPV differs from the norm in a big way by no less than 20%. Frequent children's respiration has quite understandable physiological and psychological reasons. When children worry, worry, are in a state of stress, fright, in a nervous situation, they very often react to stress with an increase in respiratory movements.
Such a tachypnea does not require correction, treatment, and usually goes away on its own as the tender children's nervous system is strengthened. If the stress is very strong, then parents can consult with a neurologist and a child psychologist.
Pathological tachypnea is always quite a serious diagnosis:
- acute or chronic infectious respiratory disease;
- bronchial asthma;
- high fever;
- traumatic brain injury, swelling of the brain and bleeding in the brain;
- pneumonia;
- tuberculosis;
- tumors in some parts of the respiratory system;
- mechanical injuries of the chest (rib fractures, cracks and displacement);
- pathologies of the cardiovascular system, congenital heart defects.
In dyspnea, superficial shallow breathing in a child is observed only during periods of increased physical activity, in moments when the child is tired and trying to catch his breath. The shortness of breath is temporary and transient. Tachypnea is permanent. If the excess of the normal respiratory rate does not disappear in a child even in a dream, this is certainly a reason to call a doctor and examine the baby for a possible disease.
What to do?
When detecting an increase in NPV in newborns, it is best to call a doctor. If the baby has other symptoms - a runny nose, cough, fever, inhale or exit became difficult, the optimal solution is to call the Ambulance.An older child can try to help yourself. A prerequisite is the absence of any additional painful symptoms.
To stop a tachypnea it is enough to take a paper bag, cut a small hole in it and invite the child to play through the bag in a game form. This will help restore gas exchange in the cells, and breathing stabilizes.
Inhale and exhale should be done only through the package, the air from the outside can not be inhaled.
A sudden increase in breathing for no apparent reason (excitement, stress, fright) is always an alarming symptom that parents should not ignore. It is important to quickly pull yourself together, calm the baby, breathe through the bag, make sure that the skin of the child has a normal color, has not changed, has not turned pale and has not appeared cyanosis. Treatment always involves treatment of the underlying disease that causes rapid breathing.
What can not be done?
Parents should not try to give the child with frequent breathing medicine. No pills and drops at this point can affect the individual symptom of a likely latent disease. But here it is quite possible to worsen the condition of the baby without the help of these drugs. You should not try to make a child with impaired breathing inhalation. They are not able to help, but the burn of the respiratory tract, which the crumb can get during steam inhalation, is a real threat.
It is important for parents to learn to distinguish tachypnea from the most common dyspnea.
About what the respiratory rate in a child is considered correct, see the following video.